Policy statement
Policy makers have long understood the role of hereditary risk factors and hereditary protective factors that affect mental health and mental illness. However, a substantial number of social factors have as great or greater effect on our mental health and often cause mental illnesses or exacerbate existing mental illnesses. Mental Health America’s core mission is to improve the mental health of all Americans. Thus, among other things, we are committed to the prevention of mental illnesses. If we are to achieve these goals we must identify, research and address the Social Driversi of Mental Health (SDOMH). The graphic below illustrates the social factors that influence mental health and the risk of mental illnesses.ii
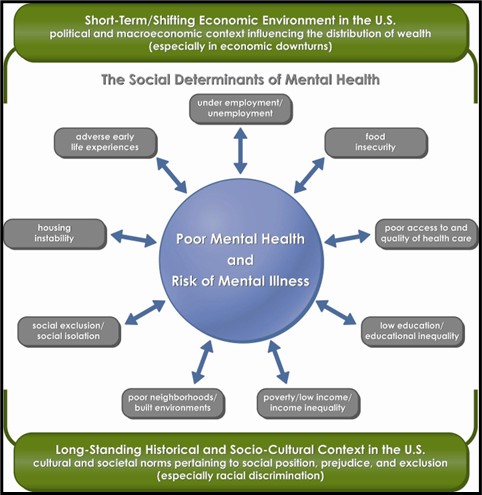
Many of these risk factors are long-standing and difficult-to-solve problems that are rooted in economic inequality and social stigmas that disproportionately affect communities of color and other marginalized groups such as the LGBTQIA+iii community. Additionally many individuals will have more than one risk factor and we must take into account the ways in which these factors intersect. In order to improve the mental health of people in America, we must have a mental health system that is responsive to the diversity of our country by providing culturally and linguistically appropriate care. Mental health advocates and providers must also, in ways that are consistent with their expertise, work with others to address the risk factors directly.
Discussion
What follows is a discussion of some of the social drivers of mental health, the ways in which these factors have an effect on mental health and proposals for actions to address these factors. While we will discuss each factor separately, that these factors interact with each other cannot be overemphasized. It is particularly important to emphasize the ways in which various forms of discrimination and social exclusion worsen outcomes in every dimension.
Poverty
The rate of poverty in America is substantial and significantly higher than other economically developed countries.iv Poverty results in or worsens every other factor effecting mental health: housing insecurityv, lack of nutritious food, bad health care and increased exposure to violence, environmental pollution and adverse childhood experiences. Poverty also directly effects the availability and quality of mental health services. The largest funder of mental health services in each of the fifty states is Medicaid, the only health care funder for most poor people State Medicaid plans provide lower reimbursement rates to mental health care providers than are paid by Medicare or private insurance.vi This reduces the availability of mental health services for those who depend on Medicaid. Many providers simply refuse to serve persons on Medicaid. As a result, many low-income areas, both urban and rural, are mental health deserts. Moreover, many indigent people, including many immigrants, are not enrolled in Medicaid and may not be eligible to enroll.vii It is extremely difficult for persons without any third-party health care payer to obtain adequate and humane mental health services.viii
Racism, Sexism, Homophobia and Other Forms of Discrimination and Social Exclusion
Like poverty, discrimination and social exclusion result in or worsen every other factor effecting mental health. African-Americans and other persons of color are more apt to experience poverty, housing insecurity, a lack of nutritious food, bad health care and increased exposure to violence, environmental pollution and adverse childhood experiences. Persons of colorix and those whose primary language is not Englishx are more apt to have undiagnosed or misdiagnosed mental illnesses, which directly and negatively affect their ability to receive adequate mental health services.
Members of the LGBTQIA+ community face distinctive mental health challenges rooted in discriminatory actions, societal biases, discrimination, and lack of understanding.xi These challenges, coupled with other daily stressors, can elevate the risk of mental health considerations. One imperative is to provide affirming support systems, access to specialized healthcare, and a culture of inclusivity and acceptance. Through education and open dialogue, inclusive understanding emerges for individuals, irrespective of their gender or sexual identity, so that they can thrive mentally and emotionally.
Safe and Secure Housing
As documented in MHA’s Position Statement: “Housing First and Supportive Housing”,xii the lack of safe and secure housing worsens mental health and exacerbates existing mental illnesses. Moreover, it is quite difficult to provide adequate and humane mental health services to persons who are unhoused. This often creates a downward spiral in which mental illness may lead to homelessness which worsens the mental illness and makes it harder to treat and harder for the person to obtain housing.
Adequate and Nutritious Food
The lack of adequate nutrition plays a substantial role in mental illnesses.xiii Additionally, poor nutrition may create or exacerbate physical illnesses such as diabetes and hypertension. These illnesses in turn create additional stress leading which worsens mental health outcomes. Persons with untreated mental illness often find it harder to maintain a consistently healthy diet worsening both physical and mental health outcomes.xiv
Quality Health Care
“Of all the forms of inequality, injustice in health care is the most shocking and inhumane.”xv Quality health care is not available to many people in the United States. Persons with mental illnesses face many barriers to health care including the fact the persons with serious untreated mental health conditions are less apt to have private health insurance or Medicare and are more apt to either rely on Medicaidxvi or have no insurance at allxvii There is a direct correlation between mental health and physical health. Poor physical health has a negative effect on mental health and poor mental health has a negative effect on physical health.xviii
Maternal Health and Reproductive Autonomy
The United States continues to face significant disparities in maternal health outcomes, with historically marginalized communities enduring the worse of these inequities. Geographical barriers, lack of healthcare infrastructure, limited insurance coverage, racial and ethnic biases, and decreased access to educational and economic attainment all limit access to quality maternal care.xix
African American women are particularly at risk of receiving inadequate pregnancy and postpartum care, including misdiagnosis and delayed treatment. As a result African American women experience higher rates of mortality and morbidity during pregnancy and childbirth, preterm births and neonatal deaths. As with other healthcare disparities, these outcomes dramatically worsen mental health outcomes.xx
The recent United States Supreme Court decision in Dobbs v. Jackson Women’s Health Organizationxxi has substantially reduced the ability of pregnant individuals to make reproductive choices. The decision whether to give birth is a uniquely personal and often difficult and stressful one. The impact of the elimination of reproductive autonomy can result in unsafe and potentially life-threatening decision forcing pregnancies, causing mental unwellness, self-harm and impacting overall physical health care. Individuals who were not able to access abortion were three times more likely to be unemployed, four times more likely to live below the federal poverty line and were more likely to experience life-threatening pregnancy complications.xxii Legal restrictions also increase shame and stigmatization surrounding the choice to terminate a pregnancy.xxiii Inevitably, these burdens negatively affect mental health.xxiv
Educational Inequality
The quality of education available to students in the United States varies widely. Poverty, race, gender, sexual identity and geography all play a substantial role in access to an adequate education.xxv This affects mental health both directly and indirectly. Persons who lack an adequate education are more apt to end up in poverty, which in turn leads to less access to mental health services. Lack of education itself also leads to worse mental health outcomes.xxvi Additionally, schools in the United States frequently lack the ability to diagnose and treat students who experience mental health problems.xxvii Untreated mental illnesses in schools leads to worse educational outcomes resulting in a downward spiral for many young people.
Violence and Community Safety
As documented in MHA’s Position Statement: “Violence: Community Mental Health Response,”xxviii violence causes mental illnesses, exacerbates existing mental illnesses and reduces the mental health of individuals and the communities in which they live. Gun violence and highly publicized mass shootings take place at high rates in the United Statesxxix. These incidents and the fear of these incidents have mental health impacts for survivors, loved ones of victims and survivors, community members in proximity to the tragedy, and society as a whole.
Survivors, first-responders, and others closely linked to violence may experience long-term psychological distress, including post-traumatic stress disorder (PTSD), depression, anxiety, and other mental health issues. In addition, mass shootings can create an atmosphere of fear and mistrust that can further exacerbate existing mental health issues. From interpersonal violence to neighborhood violence, police brutality, and hate crimes, the effects of gun and community violence include the forms of psychological distress mentioned above as well as increased substance use and suicide rates. The psychological trauma caused by gun and community violence can have long-lasting effects on individuals, families, communities, and society as a whole.
Environmental Pollution and Climate Change
Climate change and the environment are contributing factors to the SDOMH. Some of the issues include:
- Exposure to environmental pollution and toxins, limited access to green space, climate change, and extreme weather events collectively affects mental health and well-being. Environmental factors have demonstrated both physical and psychological effects on individuals, leading to a range of symptoms and mental health challenges.
- Chemical pollutants and toxins present in the airxxx, waterxxxi, and soilxxxii have resulted in damaging effects on cognitive function, contributing to impairment and a decline in mental well-being. Additionally, the presence of environmental pollutants has been associated with increased rates of anxiety, depression, and other psychological distress.xxxiii
- Research consistently shows that individuals with limited access to green spaces experience higher levels of stress, lower levels of well-being, and increased risk of chronic diseases and mental health conditions.xxxiv The absence of natural environments in urban settings contribute to feelings of isolation, heightened anxiety, and reduced resilience when faced with stressors.
- Climate change and extreme weather events can cause traumatic losses as well as disruption in people's lives. The traumatic losses experienced during climate-related disasters, such as displacement from homes, communities, and loss of employment, lead to increased stress levels and mental health exacerbation. The disruption and uncertainty caused by these events contribute to anxiety, depression, and PTSD.xxxv
- The term “solastalgia” has emerged to describe the distress and mental health challenges experienced by individuals witnessing environmental change and destruction in their familiar home environment.xxxvi Solastalgia is closely linked to a mental health issue with growing recognition, eco-anxiety. Eco-anxiety is characterized by feelings of helplessness, guilt, and despair as people struggle to come to terms with our planet’s future.xxxvii
Adverse Childhood Experiences
“Adverse childhood experiences [are] childhood events, varying in severity and often chronic, occurring in a child's family or social environment that cause harm or distress, thereby disrupting the child's physical or psychological health and development.”xxxviii Such events include experiencing or witnessing violence including experiencing or witnessing sexual assault, homelessness, physical illnesses, divorce and other forms of family disruption.xxxix Such events increase the risk of mental illnesses.xl
Call to Action
MHA urges its affiliates and other mental health advocates to:
- Support increased research aimed at understanding SDOMH with the goal of building an evidence base to drive improvement in mental health outcomes for all.
- Support an increase in screening and data collection on the effect of SDOMH on mental health and the delivery of mental health and related social services
- Support programs and practices to create a diverse mental health workforce.
- Provide SDOMH training for the entire mental health workforce.
- Collaborate with other advocates to support specific policies that combat the negative effect of SDOMH and support specific programs that promote positive mental health outcomes.xli
- Support enforcement of cultural and linguistically appropriate services (CLAS) standard to ensure equitable access to mental health services.xlii
- Support programs to insure that persons with low literacy or limited language skills have equitable access to mental health resources, tools and interventions.
i It is common to refer to the social determinants of health or mental health. MHA uses the word “drivers” rather than “determinants” because social risk factors are not immutable. We can address disparities and risk factors and can promote protective factors to improve community and individual well-being and mental health outcomes.
iii Lesbian, gay, bisexual, transgendered, queer/questioning, intersex, asexual
ivThe official poverty rate is 11.5%, meaning there are 37.9 million people living in poverty. U.S. Census Bureau; Desmond, Poverty by America (2023); Poverty Facts and Myths: America’s Poor are Worse off than Elsewhere.
vNational Alliance to End Homelessness, Income (Updated Dec. 2023); Colburn & Aldern, Homelessness is a Housing Problem (2022)
viiHow immigrants are getting healthy coverage
viii“The Behavioral Healthcare Affordability Problem” Center for American Progress (May 26, 2022)
ixBell, et al., “Misdiagnosis of African Americans with Psychiatric Issues” 107 J. Nat. Med. Assoc. pp. 25-34 (2015); Lawson, “Disparities in Mental Health Diagnosis and Treatment Among African Americans: Implications for the Correctional Systems”
xiExamples include: (1) In 2023, a record of 336 anti-LGBTQIA bills have been introduced targeting youth increasing stigma, minority stress, discrimination, bullying, violence, and chronic stress. Ramirez, M. (2023, March 2). A “crisis”: 1 in 4 Black transgender, nonbinary youths attempted suicide in previous year, study finds. USA TODAY. (2) LGBTQIA+ youth are more significantly more likely to experience depression, anxiety, suicidal thoughts, and neurodevelopmental disorders; Migdon, B. (2022, July 22). Transgender children are more likely to face mental health challenges, study says [Text]. The Hill. (3) One in four Black transgender or nonbinary youths attempted suicide last year at a rate more than twice of black cisgender peers, Ramirez, M. (2023, March 2). A “crisis”: 1 in 4 Black transgender, nonbinary youths attempted suicide in previous year, study finds. USA TODAY. 45% of LGBTQIA+ youth reported seriously considering suicide. Herron, A. (2023, April 11). Anti-Transgender Bills Take Toll on Mental Health. Fountain House.
xiiSee MHA’s Position Statement “Supportive Housing and Housing First.”
xiii“Understanding nutrition, depression and mental illnesses” Rao, et al., Indian J Psychiatry. 2008 Apr-Jun; 50(2): 77–82. Lachance and Ramsey, “Food, Mood, and Brain Health: Implications for the Modern Clinician” Mo Med. 2015 Mar-Apr; 112(2): 111–115.
xiv“How to Boost Mental Health Through Better Nutrition” American Society for Nutrition (2023)
xvMartin Luther King (1996).
xviAs discussed above in the Section on “Poverty” low Medicaid rates commonly lead to restricted access to health care. See Note v.
xviiCoombs, et al., “Barriers to healthcare access among U.S. adults with mental health challenges: A population-based study” SSM Popul Health. 2021 Sep; 15: 100847. Published online 2021 Jun 15; Roeber, et al., “Adults in poor physical health reporting behavioral Health Conditions Have Higher Health Costs” Center for Behavioral Health Statistics (2016).
xxiDobbs v. Jackson Women’s Health Org., 142 S. Ct. 2228 (2022).
xxiiTurnaway Study, Bixby Center for Global Reproductive Health & University of California San Francisco.
xxv“K-12 Disparity: Facts and Statistics” UNCF (2023); Garcia & Weiss “Education inequalities at the school starting gate.” Economic Policy Institute (2017).
xxviKondirolli 7 Sunder, “Mental health effects of education” Health Economics 2022 Oct; 31(Suppl 2): 22–39; Niemeyer, et al., “Education and mental health: Do psychosocial resources matter?” Population Health Volume 7, (April 2019); Chevalier & Feinstein, “Sheepskin or Prozac: the causal effect of education on mental health” Econstor (2006).
xxviiFor more information about the need for and lack of mental health services in schools see the following MHA Position Statements: “Early Identification of Mental Health Issues in Young People”; “Addressing the Youth Mental Health Crisis”; “Prevention of Mental Health and Substance Use Disorders in Young People”; “Discipline and Positive Behavioral Supports in Young People”.
xxviiiSee MHA’s Position Statement “Violence: Community Mental Health Response.”
xxixPew Research: What the data says about gun deaths in the U.S.; Wisevoter: Mass Shootings by Country.
xxxiMarusic, ”How contaminated water contributes to mental illness” Environmental Health News (2021).
xxxivJarosz, “Direct Exposure to Green and Blue Spaces is Associated with Greater Mental Wellbeing in Older Adults” Journal of Aging and Environment Volume 37, 2023 - Issue 4; Maas, et al., “Morbidity is related to a green living environment” J Epidemiology &Community Health (December, 2009).
xxxviAlbrecht, et al., “Solastalgia: The Distress Caused by Climate Change” ) Australas Psychiatry 2007:15 Suppl 1:S95-8; Galway, et al., “Mapping the Solastalgia Literature: A Scoping Review Study” Int. J. Environ. Res. Public Health 2019, 16(15), 2662.
xxxviiCoffey, et al., “Understanding Eco-anxiety: A Systematic Scoping Review of Current Literature and Identified Knowledge Gaps” J. Climate Change & Health (Aug. 2021); Kurth & Pihkala, “Eco-Anxiety: What it is and Why it Matters” Frontier in Psychology (Sept. 2022).
xlChapman, et al., “Adverse childhood experiences and the risk of depressive disorders in adulthood” J. of Affective Disorders Volume 82, Issue 2, 15 October 2004, Pages 217-225; Boullier & Blair, Adverse Childhood Experiences” Pediatrics & Child Health Volume 28, Issue 3, March 2018, Pages 132-137.
xliMHA urges funders such Medicare, Medicaid and private insurance to reimburse providers of peer support services and community health workers to provide assistance with SDOMH in order to improve mental health and other health outcomes.
xliiSee MHA’s Position Statement “Cultural and Linguistic Competency in Mental Health Systems.”

